Developmental Screening Step 1: Plan
This first step includes assessing the clinic’s current activities related to developmental screening, deciding what new services or changes are needed, and creating an implementation plan.
Part 1: Selecting and Training the Quality Improvement team
Each clinic will establish a quality improvement team to implement changes and to assess the impact on clinic operations and family outcomes. The make-up of the team will vary by clinic, but teams should consider representation from medical providers (physicians, nurse practitioners, and physician assistants), nurse managers, front office staff, triage nurses/medical assistants, clinic nurses, and other team members as determined by the clinics. Each team will also identify a clinic champion to guide the CQI process. The team should be introduced to the importance of developmental screening, trained on evidence-based screening tools, and instructed on using data driven decision-making for continuous quality improvement.

Champion:
The Champion leads and sustains efforts for successful implementation of developmental screening (e.g., nurse practitioner, physician). This person also provides education and support to the rest of the team.

Practice Manager/Administrator: This team member assists in determining how developmental screening fits into practice workflow, documentation, and billing.

Front Desk Staff: These members may assist by flagging patients who present for age-appropriate developmental screening and those who present for follow up. In some clinics, they may hand out screens for patients to complete in waiting rooms or provide assistance completing the screen or electronic platforms for families to access as are available for the ASQ and when using the Well Visit Planner.

Clinical Staff: Nurses and medical assistants already gather information or conduct medical assessments. Their role in developmental screening may include starting conversations about developmental screening followed by administering screens or assisting patients to access online platforms to complete the screens. Community health workers, family navigators or child development support staff can play helpful roles when available. In some clinics, they may be responsible for scoring screens or presenting results to the medical provider.

Physicians: Providers are responsible for making sure the screening is completed and scored, and results are documented in the medical record. Providers use their expertise in discussing results with the family as they offer guidance when parents need to make decisions about their child.

Parent Leader/Advisor:
Family centered care is best delivered when families lead and provide input into and play a role in practice change efforts and systems design. Identifying family leaders and ensuring their voices inform the effort is suggested. For tips on how to engage families in practice improvement efforts, explore here.
Part 2: Needs Assessment and Systems Mapping Strategies
A needs assessment is conducted to describe existing system capacities of clinics and the ability to implement developmental screening services. The systems mapping process is designed to illuminate areas of unmet needs and generate questions and priorities in terms of refining current policy and practices.
The overall objective of the mapping process is to create a visual representation of a typical patient visit flow. The team begins with a point of patient entry to the clinic and completes each layer by asking ‘What happens next’, noting at which points developmental screening or promotion occurs.
Systems mapping serves to:
- Provide a clear picture (flow chart) of the current structure and functions of the clinic.
- Identify strengths and weaknesses and enhance service delivery by prioritizing workarounds and improvement opportunities.
- Bring key team members together to support the improvement of developmental health practices.
- Highlight and prioritize data requirements for monitoring and evaluating developmental health practices.
Determine When and Where to Screen
Not all screenings must be done in the same place or administered by the same people, but a standard clinic protocol helps ensure the goal is met. Some practices have families fill out the screen in the waiting room, others in the exam room, and some even email families a blank screen before their child’s appointment. If the Well Visit Planner is used families can complete the digital tool using their phone, tablet, or computer either at home or in clinic.
Keep in mind that some families may need assistance reading and completing screening tools. When possible, provide the screen in the family’s primary language. No matter where screens are conducted, all results of the screen should always be discussed in a private space. *Across all these areas outlined below, language, literacy and equity issues should be considered and addressed.
There are pros and cons to different locations and timing during the visit:

1. A public space such as a waiting room
- Pros: Screening can be completed at home before patients arrive to the clinic or in the clinic while patients are waiting. This allows for easier scoring by the medical staff, and it can be scored before the provider sees the . If family completed and automatically scored tools are used, like the Well Visit Planner or the ASQ Online, time to score can be reduced and results can be shared ahead of time with providers and families so visit time can focus on results and needs.
Cons: When completing in the clinic, the caregiver may have reduced capability to supervise their child.

2. A private space such as an exam or triage room
- Pros: It provides lots of privacy. If required, the screening can be scored by clinical staff immediately in the room, and it can be scored before provider sees the family.
- Cons: It requires more time for clinical staff to distribute and score, if required.
3. Pre-Visit such as through electronic platforms and/or through community partnerships
- Pros: It frees up visit time to focus on promoting development and addressing identified issues. Family reflects and learns ahead of time and may be more engaged in discussions and counseling and come to the visit with their priorities identified. Community partners can be the lead to engage families that have been historically marginalized by our systems and then share results with providers having addressed family needs in areas that are appropriate (e.g. social determinants, ensuring child has a scheduled well visit, etc.). The Well Visit Planner provides data to the clinic on a data dashboard and can be shared across clinic and community-based settings.
- Cons: It requires establishing adequate communication, coordination and information sharing mechanisms. IT access gaps should be considered and addressed.
Fit the Strategies You Select into Your Workflow
Once the decision is made about where and when each screen will be performed, create a step-by-step process. Think about all the things that happen during a well-child visit, and where developmental screening will best fit in.
Example of conducing screening within the clinic (compared to pre-visit screening done at home)
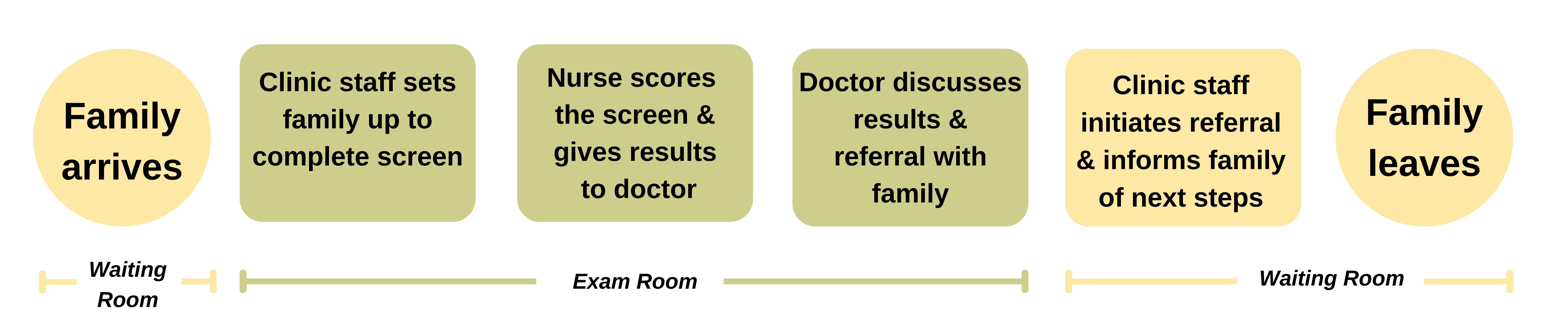
Part 3: Develop Implementation Plan
Based on results from the needs assessment, the CQI team sets goals and develops an implementation plan. The implementation plan includes a standard protocol with step-by-step instructions for all providers for screening, documentation of results in the medical record and referrals, as needed, to any service provider.
About This Resource
The overarching goal of the Child Health and Development Project (Mississippi Thrive!) has been to improve developmental health outcomes for young children through the building of a statewide developmental and behavioral health system. As part of the system build MST worked with health care providers to increase developmental screenings, connect more children to the services they need, and equip providers with materials and resources to promote developmental and behavioral health with caregivers at wellness visits. Additional work was conducted to advance more comprehensive, family-engaged, whole child approaches.
This toolkit provides information about the specific resources and approaches used to support health care providers at the University of Mississippi Medical Center to integrate developmental screening and additional approaches to engage families and conduct comprehensive screening and personalized health promotion into their pediatric practices as well as lessons learned. It was modeled after the Louisiana Developmental Screening Toolkit created by the Developmental Screening Initiative at the Louisiana Bureau of Family Health. It incorporates a Continuous Quality Improvement framework based on the clinical practice guidelines form the American Academy of Pediatrics.
This toolkit was developed by the Mississippi Thrive! Enhanced Pediatric Medical Home Services (EPMHS) team in partnership with The Child and Adolescent Health Measurement Initiative (CAHMI). The Child Health and Development Project: Mississippi Thrive! (CHDP) was a project of the University of Mississippi Medical Center’s (UMMC) Center for the Advancement of Youth (CAY) and the Social Science Research Center (SSRC) of Mississippi State University (MSU).
This project was supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award totaling $17.4 million with 0 percent financed with non-governmental sources. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government. For more information, please visit HRSA.gov today. The Child and Adolescent Health Measurement Initiative (CAHMI) is a national non-profit initiative founded in 1996 to promote the early and lifelong health of children, youth and families using family-centered health and health care quality data and improvement tools and research. The Cycle of Engagement Well Visit Planner approach was developed and is maintained by the Child and Adolescent Health Measurement Initiative (CAHMI).















